The prevalence of osteoporosis in Australia is rapidly increasing because of increased life expectancy and an ageing population. Osteoporosis affects 1 in 2 women and 1 in 3 men aged over 60 years.1-3 About 50% of fragility fractures have osteoporosis confirmed on bone densitometry criteria. The most common sites of fragility fractures are the hip, wrist and spine.1,2
Fragility fractures are associated with significant disability, increased mortality and significant cost to the health care system.4,5 Hip fracture is considered the most significant and serious type of fragility fracture. About 25% of people suffering hip fractures die within 12 months of the event, 15%–25% require long-term care and 50% require help with activities of daily living.5-8 Furthermore, people who sustain a first hip or other fragility fracture are at increased risk of subsequent fracture at all sites.4,5,9
Effective evidence-based treatments are available for patients with osteoporosis.10-12 In addition, there are Australian evidence-based guidelines on management of patients with osteoporosis with and without a fracture history.3 Furthermore, there is evidence to support targeting high-risk groups, especially people with a previous fragility fracture and older patients, as they have the greatest potential to benefit individually and are the most cost-effective groups to treat.11-13
Despite these recommendations and guidelines and the availability of appropriate treatment subsidised by the Pharmaceutical Benefits Scheme, many Australian patients with previous fragility fractures remain untreated.11,12 A large Australian study conducted in a primary care setting4 showed that less than 20% of postmenopausal women with a fracture reported receiving any specific treatment for osteoporosis, and only 8% had been investigated for osteoporosis. Western Australian data on high-risk older patients presenting to a tertiary hospital with minimal trauma fractures have shown similar low rates of treatment (< 20%) with specific antiosteoporotic therapies.14,15 Such hospital patients are considered to represent the highest readily identifiable at-risk group. An intervention level of less than 20% highlights an important lost opportunity for better population health outcomes and reduced health care costs. As reported by Zochling et al,16 patients not treated at the time of their fracture are likely to remain untreated after discharge.
One important barrier to intervention identified in two Australian studies4,14 was poor levels of awareness (50%–60%) among patients of their elevated injury risk, including those with previous fractures. Moreover, only a minority of hospital patients seemed to appreciate that osteoporosis was the underlying cause of their fragility fracture and that the osteoporosis was treatable.14
improve awareness of the risks of osteoporosis in patients with fragility fracture presenting to an emergency department (ED) or admitted to hospital;
empower patients to seek help to reduce their risk of further osteoporotic fractures;
improve awareness among hospital clinicians and general practitioners of the risks of osteoporosis in patients presenting with fragility fractures;
develop and implement a simple, user-friendly osteoporosis guideline, based on published Australian guidelines and adapted for local use, to improve the investigation and management of osteoporosis; and
encourage referral of fracture patients to a geriatrician-led, fracture liaison nurse-supported Fragile Bone Clinic for appropriate management.
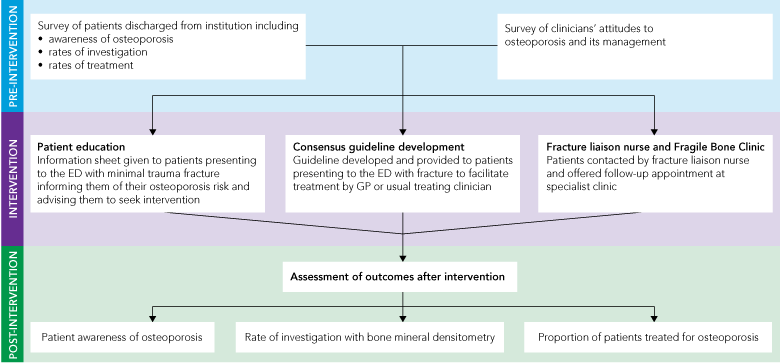
The primary target group consisted of patients presenting to the ED with fragility fractures. Secondary target groups were clinicians caring for patients within the hospital setting after fragility fracture and GPs providing care to patients after their discharge from hospital. The stages of intervention are summarised in Box 1.
Two hundred sequential patients who had experienced a fracture were surveyed to assess their awareness of osteoporosis and of the need to treat their underlying condition. This pre-assessment was conducted as part of a Bone Protection Project reported previously,14,15 which included patients discharged from the ED as well as those admitted to hospital (the present target group). The Bone Protection Project was part of a national survey that included the 200 patients discharged from the tertiary institution surveyed.
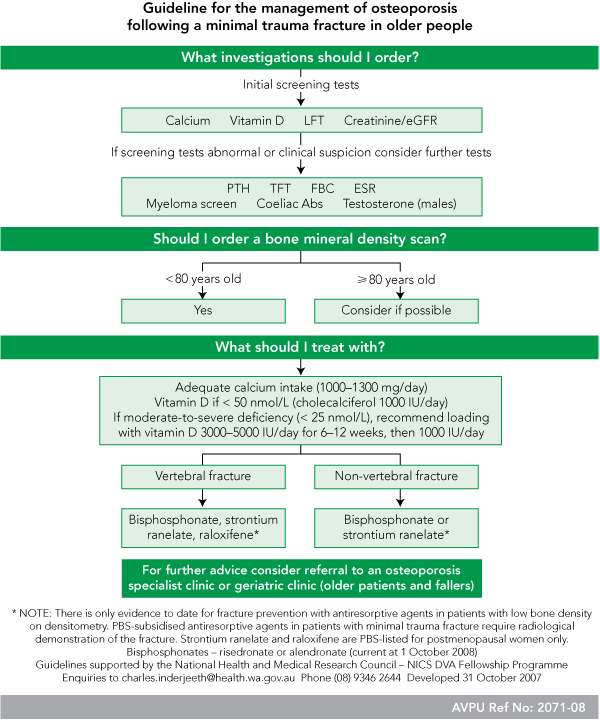
Our brief was to develop and implement a simplified and locally acceptable single-page clinical guideline to improve the management of older patients with osteoporotic fracture risk after presentation to hospital with a fracture. An extensive literature review of the evidence base for osteoporosis risk management and current guidelines was completed. A “Draft guideline for the management of osteoporosis following a minimal trauma fracture in older people” was adapted from the best available Australian guidelines.3 We invited a group of local clinicians with expertise in managing osteoporosis and representatives of the target group of GPs to review and provide feedback on the first draft guideline for local use. After amendments to the first draft, the group convened a workshop to agree on the final wording and form of the guideline. This led to a final consensus guideline that was completed and emailed to all clinicians involved in the review to ensure unanimous support. The final Consensus guideline (Box 2) was endorsed by the hospital medical executive for implementation in the clinical service.
The results of the pre-intervention survey of clinicians are presented in Box 3. Most GPs indicated that they reviewed their patients after fracture presentation to the ED (239/306 [78%]), informed them about their risk of osteoporosis (257/306 [84%]), and considered it their responsibility to investigate and manage this risk with the patient (259/306 [85%]). Most clinicians indicated that they would use simple guidelines if available.
The results of the patient surveys and audits of clinical management before and after the multimodal intervention are summarised in Box 4. Despite clinicians’ pre-intervention intentions to manage osteoporosis risk proactively, the baseline results in Box 4 show a low level of patient awareness, a low rate of investigation by bone mineral densitometry and other relevant investigations, and a lower than expected uptake of treatment. After the intervention, all of these outcome measures improved. Investigations with bone mineral densitometry increased from 6/200 (3%) to 39/87 (45%). The number of patients receiving calcium and vitamin D supplementation increased from 24/200 (12%) (for both supplements) to 29/87 (33%) and 32/87 (37%), respectively. Initiation of specific treatments increased from 12/200 (6%) to 26/87 (30%), and 35/87 patients (40%) indicated awareness of their risk. Patients identified the main prescribers of their osteoporosis treatments as GPs (52%), geriatricians (30%) and ED doctors (13%).
We also reviewed the rate of referral of all eligible patients to the Fragile Bone Clinic over the period 1 January to 30 September 2008 as an outcome (Box 5). Of the 569 patients aged 65 years or over presenting to the ED with fragility fractures, 194/569 (34%) were discharged directly from the ED and deemed eligible for referral to the Fragile Bone Clinic. Of the patients eligible for referral to the clinic, 51/194 (26%) were referred. This compared favourably with the low referral rate of 20/500 (4%) in the two calendar years before the project was implemented. When patients were contacted by the fracture liaison nurse and offered review at the clinic, 84% accepted an appointment.
Previous studies have confirmed that single strategies, including providing information to patients and implementing guidelines alone, are ineffective in improving treatment.17-19 Our project used a multimodal and multidisciplinary approach to improving awareness and management of osteoporosis risk. The focus was on empowering patients by providing easy-to-understand information and assisting clinicians by providing simple, easy-to-follow guidelines. To overcome the issue of time constraints on medical practitioners directly involved in patient care, allied health staff and other medical practitioners, including geriatricians with an explicit mandate to manage osteoporosis risk, cooperated to facilitate patient identification and management.
On a promising note, the majority (84%) of those referred agreed to be reviewed in the clinic for osteoporosis management when contacted by the fracture liaison nurse. The value of a fracture liaison service that actively identifies and proactively encourages patients to seek assessment has also been demonstrated in previous studies.20-24 One strategy that should be considered in future is to contact all patients presenting to the ED with a fracture to offer them advice and follow-up and provide multimodal care, as described here and in a study by Bogoch et al.22
3 Results of clinician survey before the intervention
Request bone mineral densitometry to assess patient’s osteoporosis |
|||||||||||||||
Feel a responsibility to investigate patients for osteoporosis |
|||||||||||||||
Received 24 December 2009, accepted 2 May 2010
- Charles A Inderjeeth1
- Denise A Glennon1
- Kate E Poland1
- Katherine V Ingram1
- Richard L Prince1
- Victoria R Van1
- C D’Arcy J Holman2,3
- 1 Osborne Park Hospital Program, North Metropolitan Area Health Service, Perth, WA.
- 2 School of Population Health, University of Western Australia, Perth, WA.
- 3 Australian Centre for Economic Research on Health, University of Western Australia, Perth, WA.
We wish to thank the following for their contribution to our project: the National Health and Medical Research Council’s National Institute of Clinical Studies and Australian Department of Veterans’ Affairs Fellowship Program; the North Metropolitan Area Health Service, Perth (Sir Charles Gairdner Hospital, Osborne Park Hospital and area rehabilitation and aged care staff); and physicians and general practitioners involved in developing the consensus guidelines.
Denise Glennon has received speaker fees from Sanofi-Aventis and Servier.
- 1. World Health Organization. Prevention and management of osteoporosis. Geneva: WHO, 2004. (WHO Technical Report Series No. 921.)
- 2. Access Economics. The burden of brittle bones: costing osteoporosis in Australia. Canberra: Access Economics for Osteoporosis Australia, 2001.
- 3. Sambrook PN, Seeman E, Phillips SR, Ebling PR. Preventing osteoporosis: outcomes of the Australian Fracture Prevention Summit. Med J Aust 2002; 176 (8 Suppl): S1-S16. <MJA full text>
- 4. Eisman J, Clapham S, Kehoe L; Australian BoneCare Study. Osteoporosis prevalence and levels of treatment in primary care: the Australian BoneCare Study. J Bone Miner Res 2004; 19: 1969-1975.
- 5. Cooper C. The crippling consequences of fractures and their impact on quality of life. Am J Med 1997; 103 (2 Suppl): 12S-19S.
- 6. Chilov MN, Cameron ID, March LM. Evidence-based guidelines for fixing broken hips: an update. Med J Aust 2003; 179: 489-493. <MJA full text>
- 7. Scaf-Klomp W, Sanderman R, Ormel J, et al. Depression in older people after fall-related injuries: a prospective study. Age Ageing 2003; 32: 88-94.
- 8. Nguyen TV, Center JR, Eisman JA. Osteoporosis: underrated, under diagnosed and undertreated. Med J Aust 2004; 180 (5 Suppl): S18-S22. <MJA full text>
- 9. Klotzbuecher CM, Ross PD, Landsman PB, et al. Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. J Bone Miner Res 2000; 15: 721-739.
- 10. Delmas PD. Treatment of osteoporosis. Lancet 2002; 359: 2018-2026.
- 11. Brooks P, Hooper M, Smallwood R. Bone and joint diseases: prevention and control. Med J Aust 2004; 180 (5 Suppl): S4-S5. <MJA full text>
- 12. Philips P, Braddon J. Osteoporosis — diagnosis, treatment and management. Aust Fam Physician 2004; 33: 111-119.
- 13. Seeman E, Eisman JA. MJA Practice Essentials 7: Treatment of osteoporosis: why, whom, when and how to treat. Med J Aust 2004; 180: 298-303. <MJA full text>
- 14. Inderjeeth CA, Glennon D, Petta A. Study of osteoporosis awareness, investigation and treatment of patients discharged from a tertiary public teaching hospital. Intern Med J 2006; 36: 547-551.
- 15. Teede HJ, Jayasuria IA, Gilfillan CP. Fracture prevention strategies in patients presenting to Australian hospitals with minimal-trauma fracture: a major treatment gap. Intern Med J 2007; 37: 674-679.
- 16. Zochling J, Schwarz J, March L, Sambrook P. Is osteoporosis undertreated after minimal trauma fracture [letter]? Med J Aust 2001; 174: 663-664.
- 17. Gross P, Greenfield S, Cretin S, et al. Optimal methods for guideline implementation: conclusions from Leeds Castle meeting. Med Care 2001; 39 (8 Suppl 2): II85-II92.
- 18. Grol R, Wensing M, Eccles M. Improving patient care: the implementation of change in clinical practice. Sydney: Elsevier, 2005.
- 19. Grol R. Between evidence-based practice and total quality management: the implementation of cost-effective care. Int J Qual Health Care 2000; 12: 297-304.
- 20. McLellan AR, Gallacher SJ, Fraser M, McQuillan C. The fracture liaison service: success of a program for the evaluation of patients with osteoporotic fracture. Osteoporos Int 2003; 14: 1028-1034.
- 21. Kimber CM, Grimmer-Somers KA. Evaluation of current practice: compliance with osteoporosis clinical guidelines in an outpatient fracture clinic. Aust Health Rev 2008; 32: 34-43.
- 22. Bogoch E, Elliot-Gibson V, Beaton D, et al. Effective initiation of osteoporosis diagnosis and treatment for patients with a fragility fracture in an orthopaedic environment. J Bone Joint Surg Am 2006; 88: 25-34.
- 23. Tosi L, Gliklich R, Kannan, K, Koval K. The American Orthopaedic Association’s “own the bone” initiative to prevent secondary fractures. J Bone Joint Surg Am 2008; 90: 163-173.
- 24. Van Helden S, Cauberg E, Geusens P, et al. The fracture and osteoporosis outpatient clinic: an effective strategy for improving implementation of an osteoporosis guideline. J Eval Clin Pract 2007; 13: 801-805.





Abstract
Objective: To implement and evaluate a multimodal intervention to improve osteoporosis treatment in patients with a fragility fracture.
Design, setting and participants: Strategies to improve the management of patients discharged from an emergency department after presentation with fragility fracture were implemented prospectively in a large tertiary public hospital. Patients were surveyed by post to assess their awareness of osteoporosis and of the need for treatment. General practitioners and hospital clinicians completed an online questionnaire about their attitudes to osteoporosis and its management. A simplified consensus guideline was developed for local use. Our study was conducted between 1 October 2007 and 31 October 2008.
Main outcome measures: Rates of referral of patients for osteoporosis review; rates of investigation and treatment.
Results: Although most GPs (259/306 [85%]) accepted that it was their responsibility to assess and treat their patients and inform them of their osteoporosis risk, only 35/87 patients (40%) indicated awareness of their risk. After implementation of our project, the rate of bone mineral densitometry investigations improved from 6/200 (3%) to 39/87 (45%) (P < 0.05). The number of patients receiving calcium and vitamin D supplementation increased from 24/200 (12%) (for both supplements) to 29/87 (33%) and 32/87 (37%), respectively (P < 0.05). Initiation of specific treatments increased from 12/200 (6%) to 26/87 (30%) (P < 0.05). Referral of eligible patients to the Fragile Bone Clinic for osteoporosis review improved from 20/500 (4%) to 51/194 (26%). After being contacted by a fracture liaison nurse, 84% of these patients presented for osteoporosis review in the clinic.
Conclusions: A major key to improving osteoporosis management is to actively identify all patients at risk and proactively engage and encourage them to seek assessment and management. A multimodal strategy involving a dedicated fracture liaison nurse may offer the greatest potential for improving education and patient follow-up and treatment.