In 1973, Hilde Bruch observed that obese children tended to belong to families characterised by a domineering, overprotective mother, a weak father, and a lack of responsiveness, warmth, and support towards the obese child.1 Later, studies also suggested that childhood obesity may be associated with some specific family characteristics, such as family cohesion, conflict, disorganisation, a lack of interest in social and cultural activities,2,3 and parental neglect.4 Other studies, however, have failed to support the hypothesis that obese children come from families displaying such dysfunctional traits.5,6 Thus, no clear pattern of family dynamics has consistently been associated with obesity.
The role of the family has implications for the treatment of obese children — family-based treatment programs for obese children are based on the theory that parenting style, family functioning, and the home environment are key factors.7-9 There is evidence of the long-term effectiveness of this approach.7
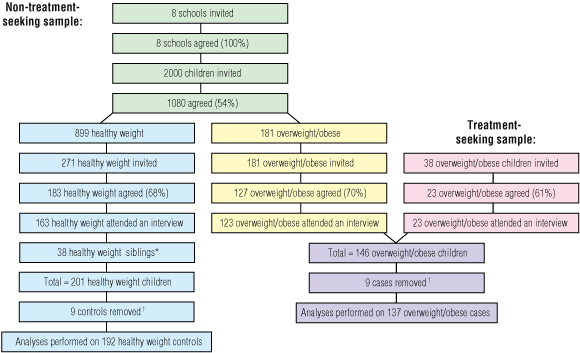
Participants for the GAD Study were recruited in two ways (Box 1).
A non-treatment-seeking sample of overweight and obese children was recruited from eight randomly selected primary schools in the Perth metropolitan area. All children at these schools took home an information sheet inviting them to be weighed and measured at school. All children with parental consent (n = 1080; 54%) who were present at the schools during the site visit were weighed in light clothing and without shoes with regularly calibrated digital medical scales (Tanita, Chicago, Ill, USA), and had their height measured with a regularly calibrated portable Harpenden stadiometer (Holtain Ltd, Crymych, UK) using the stretch technique (to the nearest millimetre). All measures were assessed twice, with the mean score recorded. Body mass index (BMI = weight [kg]/height [m]2) was calculated for each child. Children were classified as healthy weight, overweight or obese using Cole and colleagues’ age- and sex-specific overweight and obese BMI cut-offs for children.10 All children classified as overweight or obese (n = 181) were invited to participate in the prospective phase of the GAD Study (regardless of whether they were siblings of others in that group), and 127 (70%) agreed to participate; 123 of these attended the assessment interview.
Participating children and their mothers attended separate assessment interviews.
All children and their mothers were (re)weighed and (re)measured. Age- and sex-specific BMI z scores were calculated for the children using the United States Centers for Disease Control and Prevention 2000 reference data.11 Child BMI z scores were used in all analyses.
The family’s socioeconomic status was measured by maternal education level and total family income. Codes from the Socio-Economic Indexes for Areas (SEIFA), which includes an Index of Advantage/Disadvantage,12 were also obtained, based on residential address.
Depression Anxiety Stress Scales (DASS): The DASS is a set of three self-report scales designed to measure depression (dysphoria, hopelessness, devaluation of life, self-deprecation, lack of interest/involvement, anhedonia, and inertia), anxiety (autonomic arousal, skeletal muscle effects, situational anxiety, and subjective experience of anxious affect) and stress (difficulty relaxing, nervous arousal, and being easily upset/agitated, irritable/overreactive and impatient).13 Mothers rated the extent to which they had experienced each state over the previous week.
McMaster Family Assessment Device (FAD): The General Functioning Scale (12 items) of the FAD14 was administered to all mothers. This subscale assesses the overall health/pathology of the family. Mothers rated their agreement or disagreement with how well items described their family (eg, “We don’t get along well together”).
Parenting Scale: The 30-item Parenting Scale is designed to measure dysfunctional discipline practices.15 Paired extremes of discipline strategies form the anchors for a seven-point scale (eg, “When my child misbehaves, I raise my voice or yell” versus “When my child misbehaves, I speak to my child calmly”).
Life events scale: Mothers assessed recent negative life events using the List of Threatening Experiences,16 which includes 12 categories of negative life events (eg, illness, death of a close friend or relative, unemployment).
Rosenberg Self-Esteem Scale: This brief unidimensional measure of global self-esteem consists of 10 statements related to overall feelings of self-worth or acceptance.17 Items are summed to derive an overall score ranging between 10 and 40, with higher scores indicating higher maternal self-esteem.
In univariate models, increasing child BMI z score was found to be significantly associated with higher maternal BMI, an increasing likelihood of belonging to a single-parent family, fewer people living in the home, increasing social disadvantage (all P < 0.01), lower annual family income and fewer years of maternal education (both P < 0.05) (Box 2).
In a multivariate model, maternal BMI and family structure (single- or two-parent family) were the only factors significantly associated with child BMI z score (P < 0.01 and P < 0.05, respectively) (Box 2). There were no significant main or interaction effects of age group or sex.
Box 3 shows the results stratified by treatment-seeking (n = 23) and non-treatment-seeking (n = 114) overweight and obese children, both before and after adjusting for child BMI z score. Compared with mothers of non-treatment-seeking children, mothers of treatment-seeking children had significantly higher BMIs and reported significantly lower annual family incomes. Families of treatment-seeking children were more socially disadvantaged, according to the SEIFA index. However, after controlling for child BMI z score, these differences disappeared. There was also a trend for mothers of the treatment-seeking children to report higher levels of depression than mothers of the non-treatment-seeking children. This difference remained after adjusting for child BMI z score.
Using a range of well known and replicable measures of specific maternal and family characteristics, we found that having an overweight mother and coming from a single-parent (single-mother) family increased the likelihood of a child being overweight or obese. These findings are consistent with the results of a previous study conducted with a random sample of 1581 Australian school children aged 7–15 years,18 which found that having parents, especially mothers, who were overweight increased the risk of children being overweight.
However, some early research suggested that obese children tend to come from dysfunctional families,2,3 where “dysfunctional” described traits such as family conflict, disorganisation and parental neglect.
The discrepancy between the earlier studies and more recent studies of family functioning in relation to childhood obesity may reflect a temporal change. In developed countries, the prevalence of obesity among young people has increased dramatically over the past 10 years.19 Twenty to 30 years ago, when childhood obesity was significantly less prevalent, it may have been that obese children did come from relatively unsupportive family environments. Now that childhood obesity is more widespread, the problem is not confined to families with these problems.
Limitations of our study include its cross-sectional nature and omission of some aspects of family functioning, such as family communication patterns or the child’s perceived level of parental support. We are also unable to comment on the relationship between family functioning and obesity in single-father families, as there were too few of these for statistical analysis. In addition, it is important to acknowledge the possibility of a non-response bias. Families experiencing high levels of stress, maternal psychopathology or poor general functioning may have been less likely to participate in the study, thereby restricting the range of values on our measure of family functioning. However, our distribution of FAD scores suggested that the range of values was comparable to that reported in previous studies.20
2 Predicted effects of family and maternal factors on child body mass index (BMI) z scores
Family structure: single-parent family (v two-parent family) |
|||||||||||||||
|
SEIFA = Socio-Economic Indexes for Areas.12 DASS = Depression Anxiety Stress Scales. FAD = Family Assessment Device. | |||||||||||||||
3 Comparison of treatment-seeking and non-treatment-seeking overweight and obese children by family and maternal factors
Values are mean ± SD, unless otherwise indicated. BMI = Body mass index. SEIFA = Socio-Economic Indexes for Areas.12 DASS = Depression Anxiety Stress Scales. FAD = Family Assessment Device. | |||||||||||||||
- Lisa Y Gibson1
- Susan M Byrne1,2
- Elizabeth A Davis3
- Eve Blair1
- Peter Jacoby1
- Stephen R Zubrick1,4
- 1 Division of Population Sciences, Telethon Institute for Child Health Research, Centre for Child Health Research, University of Western Australia, Perth, WA.
- 2 School of Psychology, University of Western Australia, Perth, WA.
- 3 Department of Endocrinology and Diabetes, Princess Margaret Hospital for Children, Perth, WA.
- 4 Centre for Developmental Health, Curtin University of Technology, Perth, WA.
This research is funded by Healthway, HBF, and the Raine Medical Foundation. We would like to acknowledge the schools, children and parents that have given their valuable time to participate in the study. We would also like to acknowledge the contributions of our colleagues, Katie Watts, Felicity Watt, Debbie Blumberg, Alisha Thompson, Lana Bell and Karina Allen.
None identified.
- 1. Bruch H. Eating disorders: obesity, anorexia nervosa, and the person within. New York: Basic Books, 1973.
- 2. Banis HT, Varni JW, Wallander JL, et al. Psychological and social adjustment of obese children and their families. Child Care Health Dev 1988; 14: 157-173.
- 3. Beck S, Terry K. A comparison of obese and normal-weight families’ psychological characteristics. Am J Fam Ther 1985; 13: 55-59.
- 4. Lissau I, Sorensen TI. Parental neglect during childhood and increased risk of obesity in young adulthood. Lancet 1994; 343: 324-327.
- 5. Kinston W, Loader P. Eliciting whole-family interaction with a standardised clinical interview. J Fam Ther 1984; 6: 347-363.
- 6. Mendelson BK, White DR, Schliecker E. Adolescents’ weight, sex, and family functioning. Int J Eat Disord 1995; 17: 73-79.
- 7. Epstein LH, Valoski A, Wing RR, McCurley J. Ten-year follow-up of behavioural, family-based treatment for obese children. JAMA 1990; 264: 2519-2523.
- 8. Golan M, Weizman A, Apter A, Fainaru M. Parents as the exclusive agents of change in the treatment of childhood obesity. Am J Clin Nutr 1998; 67: 1130-1135.
- 9. Israel AC, Stolmaker L, Sharp JP, et al. An evaluation of two methods of parental involvement in treating obese children. Behav Ther 1984; 15: 266-272.
- 10. Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240-1243.
- 11. Ogden CL, Kuczmarski RJ, Flegal KM, et al. Centers for Disease Control and Prevention 2000 growth charts for the United States: improvements to the 1977 National Center for Health Statistics version. Pediatrics 2002; 109: 45-60.
- 12. Australian Bureau of Statistics. Census of population and housing: socio-economic indexes for areas (SEIFA), Australia, 2001. Canberra: ABS, 2003. (ABS Cat. No. 2033.0.30.001.)
- 13. Lovibond SH, Lovibond PF. Manual for the Depression Anxiety Stress Scales. Sydney: Psychology Foundation of Australia, 1995.
- 14. Epstein NB, Baldwin LM, Bishop DS. The McMaster Family Assessment Device. J Marital Fam Ther 1983; 9: 171-180.
- 15. Arnold DS, O’Leary SG, Wolff LS, Acker MM. The Parenting Scale: a measure of dysfunctional parenting in discipline situations. Psychol Assess 1993; 5: 137-144.
- 16. Brugha T, Bebbington P, Tennant C, Hurry J. The List of Threatening Experiences: a subset of 12 life event categories with considerable long-term contextual threat. Psychol Med 1985; 15: 189-194.
- 17. Rosenberg M. Society and the adolescent self-image. Revised ed. Middletown, Conn: Wesleyan University Press, 1989.
- 18. Wang Z, Patterson CM, Hills AP. Association between overweight or obesity and household income and parental body mass index in Australian youth: analysis of the Australian National Nutrition Survey, 1995. Asia Pac J Clin Nutr 2002; 11: 200-205.
- 19. Booth ML, Chey T, Wake M, et al. Change in the prevalence of overweight and obesity among young Australians, 1969–1997. Am J Clin Nutr 2003; 77: 29-36.
- 20. Byles J, Byrne C, Boyle MH, Offord DR. Ontario Child Health Study: reliability and validity of the general functioning subscale of the McMaster Family Assessment Device. Fam Process 1988; 27: 97-104.





Abstract
Objective: To investigate the relationship between a child’s weight and a broad range of family and maternal factors.
Design, setting and participants: Cross-sectional data from a population-based prospective study, collected between January 2004 and December 2005, for 329 children aged 6–13 years (192 healthy weight, 97 overweight and 40 obese) and their mothers (n = 265) recruited from a paediatric hospital endocrinology department and eight randomly selected primary schools in Perth, Western Australia.
Main outcome measures: Height, weight and body mass index (BMI) of children and mothers; demographic information; maternal depression, anxiety, stress and self-esteem; general family functioning; parenting style; and negative life events.
Results: In a multilevel model, maternal BMI and family structure (single-parent v two-parent families) were the only significant predictors of child BMI z scores.
Conclusion: Childhood obesity is not associated with adverse maternal or family characteristics such as maternal depression, negative life events, poor general family functioning or ineffective parenting style. However, having an overweight mother and a single-parent (single-mother) family increases the likelihood of a child being overweight or obese.