Abstract
Objective: To investigate possible HIV transmission among prison inmates.Setting: A prison system in an Australian State.
Participants: 13 ex-prisoners and their prison contacts.
Methods: Ex-prisoners who claimed to have been infected with HIV in prison and their prison contacts were interviewed about HIV risk behaviour. Entries in prison and community medical records were used by a three-member expert panel to establish the likelihood of primary HIV infection and its possible timing and location.
Main outcome measures: Determination of whether HIV infection probably occurred in prison.
Results: There was a very high probability that at least four of 13 ex-prisoners investigated acquired HIV in prison from shared injection equipment. Another two ex-prisoners most probably acquired HIV infection outside prison. The location of infection for the remaining seven could not be determined.
Conclusions: HIV transmission in prison has substantial public health implications as most drug-using prisoners soon return to the community. HIV prevention strategies known to be effective in community settings, such as methadone maintenance treatment and syringe exchange schemes, should be considered for prisoners.
Introduction
HIV transmission in prison has been reported in the United States,1 Scotland2 and Australia.3 The infrequency of these reports has led to a belief that HIV transmission occurs rarely among inmates. A more likely explanation is that confirmation of HIV transmission is more difficult in prisons than community settings.4
Multiple and powerful factors conducive to high HIV incidence are found in prisons. These include that:
- HIV prevalence is generally several times higher in prisons than in surrounding communities because of the considerable over-representation of injecting drug users (IDUs) among prisoners;5
- reports of syringe sharing with multiple injectors are still common in prisons but now rare in community settings;6
- HIV infection has been associated with imprisonment in France7 and Spain;8 and
- incidence of hepatitis C among IDUs incarcerated twice within a 12-month period was double that among IDUs who remained at liberty.9
Furthermore, HIV prevention measures, such as provision of sterile injecting equipment, condoms and methadone maintenance, are uncommon in prisons.10
Although several estimates of HIV prevalence have been conducted in correctional institutions,1,11,12 assessing the incidence of HIV transmission within a prison system poses considerably greater challenges.4 Most drug users serve short, repeated sentences. This hampers the investigation of infection outbreaks and identification of transmission location.
In an earlier Australian study,13 several IDUs claimed to have become infected with HIV in prison. Some reported symptoms indicative of primary HIV infection while incarcerated. The aim of this study was to assess, using epidemiological data, whether these IDUs or their contacts had become infected in prison. A similar approach has been used to investigate an HIV outbreak in a Scottish prison.2
Methods
Index cases
The investigation took place between 1993 and 1994. Seven IDUs from an earlier study13 who claimed to have acquired HIV infection in prison were recontacted. In the earlier study, respondents who had injected drugs and had recently been released from prison were recruited from methadone units, hostels for ex-prisoners or drug injectors, probation offices, syringe exchange schemes, local media advertisements, AIDS organisations and via street networking.13
Prison contacts
We traced prison contacts nominated by these seven people through the state methadone registry, AIDS services, drug users' organisations, HIV physicians and the State Registry of Deaths. The contacts were inmates with whom the seven index inmates had engaged in syringe sharing, anal sex or tattooing while in prison.Assessment of HIV infection
HIV infection was assessed by an expert panel of three HIV physicians. The experts were provided with dates of entry to and exit from prison, HIV test results, symptoms recorded at the time the prisoner believed infection occurred, self-reported symptoms and self-reported risk behaviour. All dates were referenced in months from the year before the first detected case had last tested HIV negative.
Each expert independently assessed whether the recorded symptoms indicated an HIV seroconversion illness and whether the infection occurred in prison, in the community, or if the location was indeterminate. We then accepted the majority decision in each assessment.
Ethical approval
Relevant ethics committees approved the study on condition that study participants' contacts in the community following their release from prison were not traced. We were also required to alert potential study participants to the possibility of legal or other consequences of admitting drug use in prison or transmitting HIV to another person. Participation in the study required signed, informed consent.
Information which would identify the exact time and location of these possible infections has not been included, in accordance with requirements of one ethics committee.
Results
Contact tracing
Between 1993 and 1994, seven male IDUs described in a previous study13 were recontacted (subjects A, B, C, D, E, F, G). They identified 20 prison contacts: six of these contacts could not be located, six had died of AIDS (according to death certificates), and two declined to participate for fear of repercussions for transmitting HIV. The six remaining contacts (H, I, J, K, L, M) plus the seven index cases made a total of 13 ex-prisoners available for investigation (Figure).
Prison clusters
Prison records revealed two clusters (C1, C2) of six subjects in one or two prison wings. Subjects B, E, I, K and M were held in Prison 1 (population about 250 inmates) in months 22 and 23, during which time index subject B seroconverted. Subjects B, D, I, K and M were held in Prison 2 (population about 300 inmates) in months 29 and 30, during which time contact subject K seroconverted. Index participant A was not part of either cluster, but another participant reported sharing syringes with him.
Of the six deceased potential respondents, two had been part of C1 and another two had been part of C2. According to death certificates, two deceased potential respondents became infected with HIV in the year when they were held with the clusters. Cluster analysis was not possible because of the lack of records being kept on the total number of inmates held in the prison wings during the crucial times.
Self-reported risk behaviour
Eleven participants (A, B, C, E, I, K, M, D, F, G, L) reported syringe sharing in prison, with the first seven nominating another person in this series as a sharing partner. Contact participants I and M also reported receiving a tattoo in prison, and index subject C reported unprotected anal sex.
All six deceased prison contacts wereidentified by one or more participants as having shared syringes with them around the crucial periods of months 22 and 23 and months 29 and 30.
Assessment of HIV infection
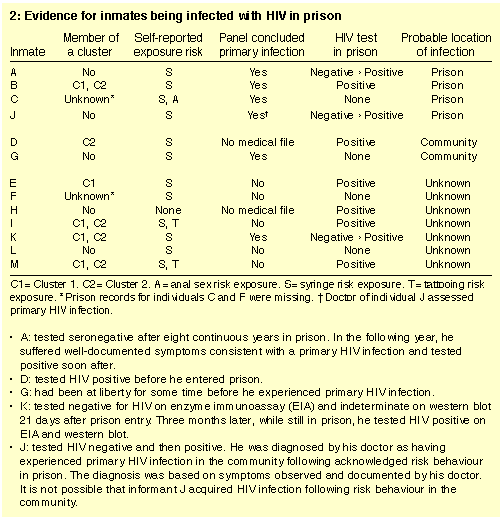
Medical file entries for 10 subjects (A, B, C, E, F, G, I, K, L, M) were reviewed by the expert panel. The experts concluded that five participants (A, B, C, G, K) had experienced primary HIV infection and that the most likely location of transmission for individuals A, B and C was in prison (Box 1). Overall, it was concluded that infection occurred in prison for four subjects and in the community for two (Box 2).
Discussion
The epidemiological evidence that individual A was infected in prison is beyond doubt: he tested negative and then positive for HIV infection after years of confinement in prison. There was strong epidemiological evidence that individuals B, C and J were also infected in prison. Individuals D and G were infected with HIV in the community. The location of infection for the remaining seven subjects (and the six deceased potential respondents) could not be determined.
Thus, on epidemiological grounds, at least four of the 13 people investigated were infected with HIV while in an Australian prison system. The most likely route of HIV transmission was shared injection equipment. These are both conservative and probabilistic assessments. It is likely that a prospective investigation of these 13 people, or even a retrospective investigation closer to the events, would have yielded a larger number of confirmed HIV transmissions in prison. However, the strength of evidence for this network and the multitude of factors conducive to HIV infection in prisons suggest that the extent of HIV transmission occurring in prisons through shared injection equipment is underestimated. A mathematical model of HIV transmission in an Australian prison system14 using values derived from empirical studies also suggests that transmission is occurring within correctional centres.
This study illustrates some of the difficulties of confirming HIV transmission in prison. We became aware of a possible outbreak by chance. Obtaining ethical approval for the study was an extremely protracted process requiring the assistance of a legal expert. Inmates were understandably wary of admitting risk behaviour because of the potentially serious consequences (as outlined in the consent form). Apart from the logistical and ethical problems of this type of research, the incubation period for HIV infection is almost as long as the average duration of a prison sentence served for drug-related offences in Australia. Consequently, many HIV infections occurring in prisons will not be detected by conventional surveillance. These factors may help to explain why so few cases of HIV transmission among inmates have been reported.
Our study differed from previous reports10 in the extent of transmission detected and the type of prisoners studied. Previous studies have investigated long term, high security prisoners, who have less opportunity to associate with other inmates and visitors to obtain drugs and consequently become infected with HIV.15 Our study found a relatively large number of incident cases considering the small sample size, the extremely low prevalence of HIV infection in the Australian prison population16 and the rapid turnover of inmates. All these factors militate against detection of HIV transmission in prison.
A limitation of the study was reliance on self-reported risk behaviour. However, we accepted self-reported data only if corroborated by another external source. Moreover, symptoms reported by informants coincided closely with medical records, supporting the validity of self-reported data.
We were precluded by ethics committee requirements from determining whether any sexual partners (and their children) were infected with HIV by participants following release from prison. This restriction prevented investigation of possible HIV transmission beyond prison to the community. However, medical files indicated that four subjects had each had an HIV-positive female sexual partner following release from prison. Two of these women, and an additional HIV-negative partner, became pregnant, with at least two pregnancies reaching full term. Medical files also indicated that at the time of the investigation two former inmates had been engaging in unprotected sex with two HIV-negative women, against the advice of their counsellors.
Existing evidence of HIV transmission among prisoners has persuaded prison authorities in few countries to implement effective prevention strategies for inmates. Confirmation of HIV infection from prison to the community may be more persuasive for authorities.
Syringe exchange, methadone and bleach programs reduce the spread of HIV in community settings,16-18 and preliminary results from these programs in prison appear promising.19-21 The paucity of data confirming HIV transmission in prison should not be regarded as adequate justification for the lack of effective HIV prevention measures within prisons. There is already sufficient information on HIV transmission between prisoners to justify rapid implementation in correctional institutions of prevention measures shown to be effective in community settings. Improved methods of monitoring the spread of HIV within prisons and from inmates to community members following release are required urgently.
Acknowledgements
We are grateful to the NSW Department of Health for funding this study. We also wish to thank David Buchanan, Andrew Carr, Ying Chun Ge, David Cooper, Anthony Cunningham, Basil Donovan, John Dwyer, Tania Sorrell and Dominic Dwyer.
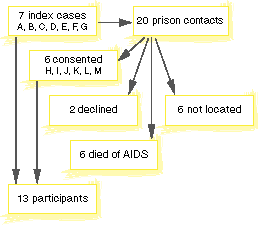
Results of tracing 20 prison contacts of seven
index cases for recruitment into the study.
References
- Brewer TF, Vlahov D, Taylor E, et al. Transmission of HIV-1 within a statewide prison system. AIDS 1988; 2: 363-367.
- Taylor A, Goldberg D, Emslie J, et al. Outbreak of HIV infection in a Scottish prison. BMJ 1995; 310: 289-292.
- Dolan K. AIDS, drugs and risk behaviour in prison: state of the art. Int J Drug Policy 1997; 8: 5-17.
- Dolan K. Why is there conflicting evidence of HIV transmission in prison? In: O'Brien O, editor. Report of the 3rd European Conference on Drug and HIV/AIDS Services in Prison. London: Cranstoun Drug Services, 1997; 19-21.
- Gaughwin MD, Douglas RM, Wodak AD. Behind bars -- risk behaviours for HIV transmission in prisons, a review. In: Norberry J, Gerull SA, Gaughwin MD, editors. HIV/AIDS and prisons conference proceedings. Canberra: Australian Institute of Criminology, 1991; 89-107.
- Crofts N, Webb-Pullman J, Dolan K. An analysis of trends over time in social and behavioural factors related to the transmission of HIV among IDUs and prison inmates. Evaluation of the National HIV/AIDS Strategy. Technical Appendix 4. Canberra: AGPS, 1996.
- Richardson C, Ancelle-Park R, Papaevangelou G. Factors associated with HIV seropositivity in European injecting drug users. AIDS 1993; 7: 1485-1491.
- Granados A, Miranda MJ, Martin L. HIV seropositivity in Spanish prisons. Presented at the VIth International AIDS Conference, San Francisco. Abstract no Th.D.116, 1990.
- Crofts N, Stewart T, Hearne P, et al. Spread of blood-borne viruses among Australian prison entrants. BMJ 1995; 310: 285-288.
- Dolan K, Wodak A, Penny R. AIDS behind bars: preventing HIV spread among incarcerated drug injectors. AIDS 1995; 9: 825-832.
- Vlahov D, Brewer TF, Castro KG, et al. Prevalence of antibody to HIV-1 among entrants to US correctional facilities. JAMA 1991; 265: 1129-1132.
- Bird AG, Gore SM, Jolliffe DW, Burns SM. Anonymous HIV surveillance in Saughton Prison, Edinburgh. AIDS 1992; 6: 725-733.
- Dolan K, Wodak A, Hall W, et al. Risk behaviour of IDUs before, during and after imprisonment. Addict Res 1996; 4: 151-160.
- Dolan K, Wodak A, Hall W, Kaplan E. A mathematical model of HIV transmission in NSW prisons. Drug Alcohol Depend 1998; 50: 197-202.
- Dye S, Isaacs C. Intravenous drug misuse among prison inmates: implications for spread of HIV. BMJ 1991; 302: 1506.
- Feachem R. Valuing the past . . . investing in the future. Evaluation of the National HIV/AIDS Strategy. 1993-94 to 1995-96. Canberra: AGPS, 1996.
- Ward J, Mattick R, Hall W. Methadone maintenance treatment and other opioid replacement therapies. Amsterdam: Harwood Academic Publishers, 1998.
- Normand J, Vlahov D, Moses LE. Preventing HIV transmission: the role of sterile needles and bleach. Washington: National Academy Press, 1995.
- Nelles J, Harding T. Preventing HIV transmission in prison: a tale of medical disobedience and Swiss pragmatism. Lancet 1995; 346: 1507-1508.
- Dolan K, Wodak A, Hall W. Methadone maintenance treatment reduces heroin injection in NSW prisons. Drug Alcohol Rev 1998; 17: 153-158.
- Dolan K, Wodak A, Hall W. A bleach program for inmates in NSW: an HIV prevention strategy. Aust N Z J Public Health 1998; 22: 838-840.
Authors' details
National Drug and Alcohol Research Centre, University of New South Wales, Sydney, NSW.
Kate A Dolan, BSc, PhD, Research Fellow.
Alcohol and Drug Services, St Vincent's Hospital, Sydney, NSW.
Alex Wodak, FRACP, FAFPHM, Director.
Reprints: Dr K A Dolan, Research Fellow, National Drug and Alcohol
Research Centre, University of New South Wales, Sydney, NSW
2052.
Email: ndarc8@unsw.edu.au
Received 8 February 2026, accepted 8 February 2026
- Kate A Dolan
- Alex Wodak
- 1.
- Brewer TF, Vlahov D, Taylor E, et al. Transmission of HIV-1 within astatewide prison system. AIDS 1988; 2: 363-367.
- 2.
- Taylor A, Goldberg D, Emslie J, et al. Outbreak of HIV infection in aScottish prison. BMJ 1995; 310: 289-292.
- 3.
- Dolan K. AIDS, drugs and risk behaviour in prison: state of the art.Int J Drug Policy 1997; 8: 5-17.
- 4.
- Dolan K. Why is there conflicting evidence of HIV transmission inprison? In: O'Brien O, editor. Report of the 3rd European Conferenceon Drug and HIV/AIDS Services in Prison. London: Cranstoun DrugServices, 1997; 19-21.
- 5.
- Gaughwin MD, Douglas RM, Wodak AD. Behind bars -- risk behavioursfor HIV transmission in prisons, a review. In: Norberry J, Gerull SA,Gaughwin MD, editors. HIV/AIDS and prisons conference proceedings.Canberra: Australian Institute of Criminology, 1991; 89-107.
- 6.
- Crofts N, Webb-Pullman J, Dolan K. An analysis of trends over time insocial and behavioural factors related to the transmission of HIVamong IDUs and prison inmates. Evaluation of the National HIV/AIDSStrategy. Technical Appendix 4. Canberra: AGPS, 1996.
- 7.
- Richardson C, Ancelle-Park R, Papaevangelou G. Factorsassociated with HIV seropositivity in European injecting drugusers. AIDS 1993; 7: 1485-1491.
- 8.
- Granados A, Miranda MJ, Martin L. HIV seropositivity in Spanishprisons. Presented at the VIth International AIDS Conference, SanFrancisco. Abstract no Th.D.116, 1990.
- 9.
- Crofts N, Stewart T, Hearne P, et al. Spread of blood-borne virusesamong Australian prison entrants. BMJ 1995; 310: 285-288.
- 10.
- Dolan K, Wodak A, Penny R. AIDS behind bars: preventing HIV spreadamong incarcerated drug injectors. AIDS 1995; 9: 825-832.
- 11.
- Vlahov D, Brewer TF, Castro KG, et al. Prevalence of antibody toHIV-1 among entrants to US correctional facilities. JAMA1991; 265: 1129-1132.
- 12.
- Bird AG, Gore SM, Jolliffe DW, Burns SM. Anonymous HIVsurveillance in Saughton Prison, Edinburgh. AIDS 1992; 6:725-733.
- 13.
- Dolan K, Wodak A, Hall W, et al. Risk behaviour of IDUs before,during and after imprisonment. Addict Res 1996; 4: 151-160.
- 14.
- Dolan K, Wodak A, Hall W, Kaplan E. A mathematical model of HIVtransmission in NSW prisons. Drug Alcohol Depend 1998; 50:197-202.
- 15.
- Dye S, Isaacs C. Intravenous drug misuse among prison inmates:implications for spread of HIV. BMJ 1991; 302: 1506.
- 16.
- Feachem R. Valuing the past . . . investing in the future.Evaluation of the National HIV/AIDS Strategy. 1993-94 to 1995-96.Canberra: AGPS, 1996.
- 17.
- Ward J, Mattick R, Hall W. Methadone maintenance treatment andother opioid replacement therapies. Amsterdam: Harwood AcademicPublishers, 1998.
- 18.
- Normand J, Vlahov D, Moses LE. Preventing HIV transmission: therole of sterile needles and bleach. Washington: National AcademyPress, 1995.
- 19.
- Nelles J, Harding T. Preventing HIV transmission in prison: a taleof medical disobedience and Swiss pragmatism. Lancet 1995;346: 1507-1508.
- 20.
- Dolan K, Wodak A, Hall W. Methadone maintenance treatment reducesheroin injection in NSW prisons. Drug Alcohol Rev 1998; 17:153-158.
- 21.
- Dolan K, Wodak A, Hall W. A bleach program for inmates in NSW: an HIVprevention strategy. Aust N Z J Public Health 1998; 22:838-840.