|
Research
End-stage renal disease in Aboriginals in New South Wales: a very
different picture to the Northern Territory
Alan Cass, Adrian G Gillin and John S Horvath
MJA 1999; 171: 407-410
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on Aboriginal health
|
| |
Abstract |
Objectives: To compare the incidence of end-stage
renal disease (ESRD) among Aboriginals in New South Wales with the
incidence among Aboriginals in the Northern Territory, and to
compare the patterns of ESRD among Aboriginals and non-Aboriginals
in NSW.
Design: Secondary data analysis of information from
unpublished and published Australia and New Zealand Dialysis and
Transplant Registry reports.
Main outcome measures: Average annual incidence of ESRD
(persons per million); form of renal replacement therapy; mortality
at 31 March 1998; patient and graft survival one and five years after
transplant.
Results: Each year in NSW, 5-17 new Aboriginal patients
are treated for ESRD. There was no increase in the average annual
incidence of ESRD among NSW Aboriginals (118 per million in 1988-1989
and 111 per million in 1996-1997), whereas incidence in the NT
increased from 255 per million to 800 per million. In NSW, ESRD was
attributed to diabetes in 32% of Aboriginal patients, compared with
13% of non-Aboriginal patients (P < 0.001). In NSW,
Aboriginal patients were younger and more likely to be female, a
pattern similar to that in the NT. The outcome of ESRD treatment is not
significantly different between Aboriginals and non-Aboriginals
in NSW.
Conclusion: There is a different pattern of incidence of
ESRD and of outcomes with treatment among Aboriginals in NSW compared
with those in the NT. A possible explanation is that the lower
incidence in NSW reflects less profound socioeconomic disadvantage
and better access to primary and specialist care.
|
| | Introduction |
Indigenous Australians experience high morbidity and mortality due
to end-stage renal disease (ESRD). In the Northern Territory, the
average annual incidence of ESRD for Aboriginals in 1988-1993 was
17.4 times that for non-Aboriginals,1 a disparity made more
apparent by age adjustment.2 The number of dialysis
treatments in the NT is doubling every two years.3 The 30 June 1996 estimate of the Indigenous population (386 049)
represented 2.1% of the total Australian population,4 but Aboriginals
constitute 5% of the Australian members of the Australia and New
Zealand Dialysis and Transplant Registry (ANZDATA).5 Whether the
increasing incidence and prevalence of renal disease is occurring in
NSW as well as nationally and in the NT has not been well documented.
The aims of our study were to document the number of new Aboriginal
patients with ESRD in NSW during 1987 to 1998 and compare recent trends
in incidence with national and NT data, and to compare for Aboriginal
and non-Aboriginal patients in NSW:
- the patterns of
aetiology of ESRD;
- the demographic characteristics at the time of being entered into
ANZDATA;
- the outcomes for individuals who were notified to the Registry
during the period 1987 to 1998; and
- patient and graft survival for those who received transplants
during the period 1987 to 1998.
|
| |
Methods |
Information was obtained from ANZDATA Annual Reports (12 and
18-21)6-10 and unpublished data
from ANZDATA. All nephrology units in Australia and New Zealand that
provide dialysis or transplant services submit detailed
six-monthly reports to ANZDATA. The reports give information
regarding new patients accepted onto treatment programs, deaths
that have occurred, and any alteration in treatment for current
patients, including changing the mode of dialysis or receiving a
transplant.
For NSW, the NT and across Australia, we analysed:
- the
number of Aboriginal patients entered into ANZDATA from 1987 to 1998
in NSW, the NT and across Australia; and
- the average annual incidence of ESRD.
For NSW only, we analysed:
- primary renal disease
diagnostic category;
- mean age;
- outcome data at 31 March 1998 for people who had been entered into
ANZDATA since 1 January 1987. Outcomes were categorised as death,
functioning transplant, haemodialysis, continuous ambulatory
peritoneal dialysis (CAPD), and loss to follow-up or having moved
interstate;
- causes of death, categorised into cardiac, vascular, infection,
social, malignancy and other;
- patient survival and graft survival for transplants performed
between 1 January 1987 to 31 March 1998.
The average annual incidence of ESRD was calculated using Australian
Bureau of Statistics (ABS) estimates and projections of the
Aboriginal and Torres Strait Islander population for the years
between actual Census counts. These estimates are based upon current
trends in fertility and mortality and take into account an increasing
propensity for people to identify themselves as being of Indigenous
origin. The definition of "Aboriginality" from both data sources
(ANZDATA and ABS) relies upon self-identification. Annual
incidence was calculated as an average for each two-year period, as
there is marked variability in the number of new patients per year, and
small absolute numbers.
Statistical analysis of demographic and outcome data was performed
using STATA 5.0.11 A t test of means
and χ2
test or Fisher's exact test of proportions were performed. Survival
analysis was performed at the ANZDATA Registry. Data were provided as
actuarial life-table estimates and the log rank test was performed.
The data were entered into STATA 5.0 and graphed.
|
| |
Results |
| |
Incidence |
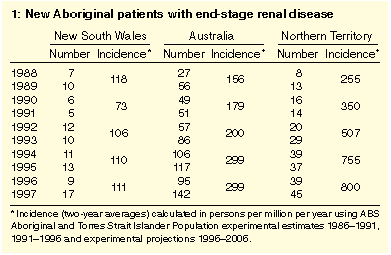
Each year in NSW, 5-17 new Aboriginal patients are treated for ESRD (Table 1). The average annual incidence of ESRD
among Aboriginals in NSW for the two years 1988-1989 was 118 per
million. This remained substantially unchanged at 111 per million in
1996-1997. During the same period the average annual incidence of
ESRD in Aboriginals across Australia increased significantly (Table 1); in the NT, the rise in incidence was
more marked. The crude incidence for non-Aboriginals in NSW was 78 per
million for 1993-1997, a slight rise from the 1980s due to increased
acceptance for dialysis of patients over the age of 65 years.
| |
Diagnostic categories | |
Diabetes, glomerulonephritis and hypertension are the most common
primary renal diseases among Aboriginals with ESRD in NSW (Table 2). Diabetes is listed as the primary
renal disease in 32% of Aboriginals, compared with 13% of
non-Aboriginals (P < 0.001). Analgesic nephropathy
affects a significantly greater proportion of the non-Aboriginal
population, mainly among females: 28% in non-Aboriginal females,
compared with 10% in Aboriginal females. No definite diagnosis was
recorded for 11% of Aboriginals, compared with 5% of non-Aboriginals
(P = 0.004).
| |
Demographics |
Significantly more Aboriginal females than males entered the ESRD
program in NSW (Table 3), the reverse
pattern to non-Aboriginals (P = 0.03). The Aboriginal
population was younger at entry to the program and there were
significantly fewer people over the age of 65 years (P <
0.001). Outcome, or patient status at 31 March 1998, was not
significantly different between the groups (P = 0.59).
However, no attempt at age or sex standardisation has been made in this
analysis.
| |
Causes of death | |
The differences between Aboriginals and non-Aboriginals in NSW in
causes of death approach statistical significance (P =
0.07). A significantly larger proportion of Aboriginals died from
cardiovascular diseases (P = 0.01). A significantly smaller
proportion of deaths were due to social reasons (P = 0.02).
| |
Patient and graft survival after transplant | |
Aboriginal patients receiving transplants in NSW during the study
period were younger (Figure 1), but
experienced lower patient survival and graft survival rates
(Figures 2a and 2b), although these differences were not significant
(Table 4).
|
| |
Discussion |
Our data show no evidence of an epidemic of renal failure among
Aboriginals in NSW, although the incidence remains higher than among
the non-Aboriginal population. Aboriginal patients in NSW with ESRD
are on average 10 years younger than non-Aboriginal patients, more
likely to be female, and more likely to have diabetes and to die of
cardiovascular disease. These features are similar to those
reported in the NT.2 However, in NSW, there is no
significant difference in outcome between Aboriginal and
non-Aboriginal patients who have been entered into the Registry
since January 1987, whereas, in the NT, survival is significantly
worse in Aboriginal than in non-Aboriginal patients.2 The
persistently high rate of withdrawal up to 1997 of NT Aboriginal
people from ESRD treatment, about 25%,3 is not present in NSW.
Our results show that diabetes, glomerulonephritis and
hypertension are the prominent primary causes of ESRD among NSW
Aboriginals. The rise in renal failure attributed to diabetes
follows a similar pattern to that noted in Aboriginals across
Australia.10 The pattern of primary
causes of renal disease is consistent between Aboriginal
populations in different States.10
Impediments to effective and culturally appropriate service
delivery to Aboriginal patients have been postulated as reasons for
poor survival and high withdrawal rates from treatment.12 Therapeutic
programs have typically removed people from their cultural and
social support networks by requiring patients to leave their land,
families and communities.13 Unlike in the NT, South
Australia and Western Australia, there are few remote,
non-urbanised communities in NSW; Aboriginals in NSW reside
predominantly in cities and rural towns.
The higher proportion of Aboriginal patients with uncertain
aetiology of their ESRD is consistent with a lower renal biopsy rate,
which may relate to late referral and lack of access to renal
specialist services. In NSW, specialist renal services are
increasingly being provided where Aboriginals live. The
Statistical Local Areas with the highest proportion of Indigenous
people are Brewarrina (53.1%), Central Darling (25.3%), Bourke
(24.5%) and Walgett (20.4%).14 CAPD training is now
occurring in some larger rural centres, and haemodialysis
facilities are provided in Bourke and Brewarrina. These
initiatives, which significantly reduce the dislocation of
patients from their community and remove impediments to the delivery
of appropriate ESRD services, may facilitate improved survival.
There is a tendency towards lower patient survival and graft survival
among NSW Aboriginals compared with non-Aboriginals, despite the
Aboriginal graft recipients' being younger. In the NT, graft and
patient survival among Aboriginals are significantly worse at one
and five years than among non-Aboriginals.2 A significant difference in
survival is not evident in the NSW data. The larger 95% confidence
intervals in the NSW Aboriginal group are a consequence of fewer
transplants being performed: 36 among Aboriginal patients,
compared with 1755 among non-Aboriginal patients. These numbers do
not provide sufficient power to detect a significant difference
between the groups.
The pattern of rapidly increasing incidence of ESRD among
Aboriginals across Australia, especially in the NT, is not seen in
NSW. Spencer et al argue that the increase in the NT is real, not due to
ageing of the Aboriginal population or improved
ascertainment.2 The reason for this
difference in incidence is not clear. It may be due to differences
between the populations in apparent predisposition to renal disease
or to differences in the prevalence of primary causes and promoters of
chronic renal disease. The epidemic of disease in the NT is not only due
to an increased prevalence of diabetes. Community screening studies
show a prevalence of significant proteinuria in marked excess of the
prevalence of diabetes or impaired glucose tolerance.2,15 In the NT,
from 1988 to 1993, the average annual incidence of ESRD not
attributable to diabetes was 350 per million per year among
Aboriginals.1 Lower incidence of ESRD in
NSW Aboriginals may reflect less profound socioeconomic
disadvantage and readier access to effective primary and specialist
care. However, there may be poor ascertainment,
particularly in rural areas of NSW. Further study is indicated to
analyse this question.
|
Acknowledgements | |
The data reported here have been supplied by the Australia and New
Zealand Dialysis and Transplant Registry. The interpretation of
these data is the responsibility of the authors and in no way should be
seen as an official policy or interpretation of the Australia and New
Zealand Dialysis and Transplant Registry.
Dr Alan Cass is the recipient of a postgraduate research scholarship
from the Centre for Kidney Research, New Children's Hospital,
Sydney.
We thank Dr Wendy Hoy, who critically reviewed the manuscript, and Dr
Zhiqiang Wang, who provided statistical advice.
|
| |
References |
- Hoy WE, Mathews JD, Pugsley DJ. Treatment of end-stage renal
disease in the Top End of the Northern Territory: 1978-93.
Nephrology 1995; 1: 307-313.
-
Hoy WE, McFarlane R, Pugsley DJ, et al. Markers for cardiovascular
and renal morbidity: expectations for an intervention programme in
an Australian aboriginal community. Clin Exp Pharmacol Physiol
1996; 23: S33-S37.
-
Spencer JL, Silva DT, Snelling P, Hoy WE. An epidemic of renal
failure among Australian Aboriginals. Med J Aust 1998; 168:
537-541.
-
Australian Bureau of Statistics. Experimental estimates of the
Aboriginal and Torres Strait Islander population. Canberra: ABS,
1998. (Catalogue No. 3230.0.)
-
Disney AP. Demography and survival of patients receiving
treatment for chronic renal failure in Australia and New Zealand:
report on dialysis and renal transplantation treatment from the
Australia and New Zealand Dialysis and Transplant Registry. Am J
Kidney Dis 1995; 25: 165-175.
-
Disney APS, Collins J, Russ GR, et al. ANZDATA Registry Report 1989.
Adelaide: Australia and New Zealand Dialysis and Transplant
Registry, 1989.
-
Disney APS, Collins J, Russ GR, et al. ANZDATA Registry Report 1995.
Adelaide: Australia and New Zealand Dialysis and Transplant
Registry, 1995.
-
Disney APS, Collins J, Russ GR, et al. ANZDATA Registry Report 1996.
Adelaide: Australia and New Zealand Dialysis and Transplant
Registry, 1996.
-
Disney APS, Collins J, Russ GR, et al. ANZDATA Registry Report 1997.
Adelaide: Australia and New Zealand Dialysis and Transplant
Registry, 1997.
-
Disney APS, Collins J, Russ GR, et al. ANZDATA Registry Report
1998. Adelaide: Australia and New Zealand Dialysis and Transplant
Registry, 1998.
-
STATA statistical software [computer program]. Version 5.0.
College Station, Texas: Stata Corporation, 1997.
-
Bennett E, Manderson L, Kelly B, Hardie I. Cultural factors in
dialysis and renal transplantation among aborigines and Torres
Strait Islanders in north Queensland. Aust J Public Health
1995; 19: 610-615.
-
Willis J. Fatal attraction: do high technology treatments for
end-stage renal disease benefit aboriginal patients in central
Australia? Aust J Public Health 1995; 19: 603-609.
-
Australian Bureau of Statistics. Census of population and
housing -- selected social and housing characteristics for
statistical local areas, New South Wales and Jervis Bay. Canberra:
ABS, 1996. (Catalogue no. 2015.1.)
-
Van Buynder PG. The epidemiology of renal disease in Aboriginal
Australians [Master of Public Health thesis]. Sydney: University of
Sydney, 1991.
(Received 12 Feb, accepted 19 Jul, 1999)
|
| | Authors' details |
Menzies School of Health Research, Darwin, NT.
Alan Cass, MB BS, FRACP, PhD student.
Department of Renal Medicine, Royal Prince Alfred Hospital, Sydney,
NSW.
Adrian G Gillin, FRACP, PhD, Staff Specialist;
John S
Horvath, MB BS, FRACP, Professor.
Reprints will not be available from the authors.
Correspondence: Dr A
Cass, Menzies School of Health Research, PO Box 41096, Casuarina, NT
0811.
alancassATmenzies.edu.au
|
| |  | | Back to text | |  | | Back to text | | 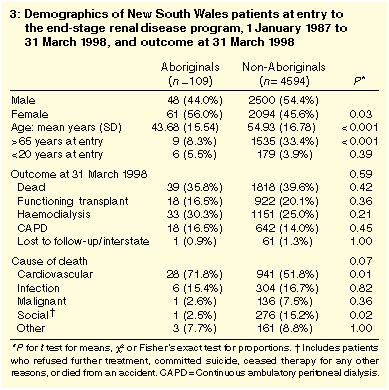 | | Back to text | |  | | Back to text | | 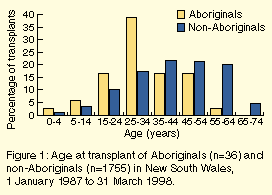 | | Back to text | | 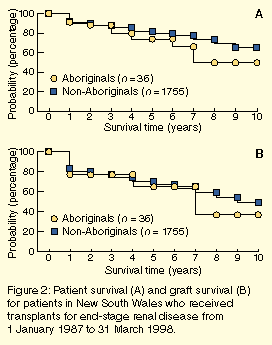 | | Back to text |
|










